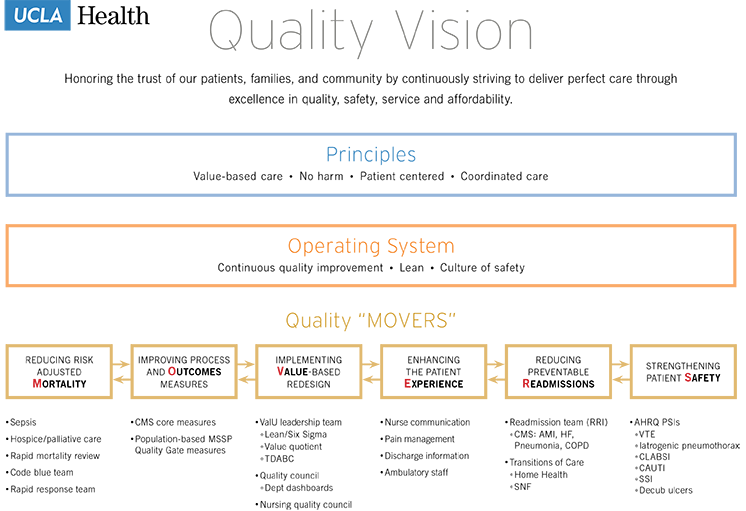
Quality Initiatives
Performance Improvement
Performance Improvement & Patient Safety Plan:
The Performance Improvement and Patient Safety Plan is a description of the organizational, multidisciplinary, and systematic performance improvement function designed to support the Mission, Values, and Philosophy of the UCLA Health System. The intent of the Performance Improvement and Patient Safety Plan is to identify the health system’s approach to improving and sustaining its performance through the prioritization, design, implementation, monitoring, and analysis of performance improvement initiatives. Moreover, the Performance Improvement and Safety Plan is an ongoing program that demonstrates measurable improvement in indicators for which there is evidence that they will improve patient outcomes, and identify and reduce medical errors.
To read the Performance Improvement & Patient Safety Plan, click here.
Just Culture:
UCLA Health practices and promotes Just Culture as the core framework for addressing patient safety related concerns. The following Just Culture presentation series has been created to provide UCLA Health staff an understanding of what Just Culture refers to in a high-consequence industry such as healthcare.
Part I:
What is Just Culture – Expected Human Behaviors – Accountability and Types of Errors – Outcome Bias
To review the slides for Just Culture Presentation Part I, click here
Part II:
Managing System Design – Role of Event Investigation
To review the slides for Just Culture Presentation Part II, click here
Part III:
The Just Culture Algorithm
To review the slides for Just Culture Presentation Part III, click here
Patient Safety: Good Catch Program
The good catch program is a formal recognition of staff and faculty who have taken action to prevent or mitigate harm brought about by “close calls”, hazardous conditions or errors.
To read about how a Good Catch is nominated, reviewed and awarded, please see the the process map or presentation.
Core Measures
SCIP:
The Surgical Care Improvement Project (SCIP) is a national partnership aimed at improving the quality and safety of surgical care by reducing post-operative complications. Originally developed by the Centers for Medicare & Medicaid Services (CMS) and the Centers for Disease Control and Prevention (CDC), the SCIP partnership is a multi-year national campaign to substantially reduce surgical mortality and morbidity.
If you have questions about SCIP please email SCIP@mednet.ucla.edu.
Data Registries
For an overview and list of data registries at UCLA please click here.
VQI
Virtual PICU System (VPS):
The Virtual PICU System or VPS is a clinical database dedicated to standardized data sharing and benchmarking among pediatric ICUs. All participants collect information on patient and hospital measures, diagnoses, interventions, discharge, organ donation, and pediatric severity of mortality scores. It has been designed to create a network of children's hospitals and other facilities offering PICU care to improve the quality of critical care for children worldwide.
Case Mix Comparative Data Program through the Children’s Hospital Association (CHA):
The Case Mix Comparative Data Program is the largest available database for children's hospitals in the United States, allowing participants access to an ever-growing wealth of information. The Case Mix program is an inpatient discharge-level database with over 7 million cases spanning more than six years and close to 90 children's hospitals. It includes custom methodologies for the most pediatric-sensitive benchmarking and grouping of populations. With over 300 data elements available for querying, the program provides a highly robust ability to examine segments of the population of interest. The Case Mix program helps target quality improvement activities, enhances hospital utilization, develops pricing strategies and supports advocacy on behalf of children’s hospitals. Hospitals may compare and benchmark with comparable peer groups within hospitals as well as all children's hospitals across the country.
Heart Failure
AMI
Stroke:
Stroke is the fourth leading cause of death in the United States and one of the leading causes of long-term disability. Stroke refers to the acute neurological impairment that follows blockage or rupture of a blood vessel supplying a specific region of the brain.
It is beneficial to classify strokes as either hemorrhagic or ischemic. Ischemic strokes account for 87 percent of all strokes, and treatment that can dramatically improve outcome is available for a certain subset of carefully screened patients.
Time is brain. For every minute an ischemic stroke is left untreated, an estimated 1.9 million neurons are destroyed. Each hour in which treatment fails to occur, the brain loses as many neurons as it does in almost 3.6 years of normal aging. The sooner treatment is started, the smaller the area of permanent damage will be and the better the quality of life the patient will have.
NSQIP:
The American College of Surgeons National Surgical Quality Improvement Program (ACS NSQIP) is a quality improvement database that allows hospitals to focus their quality improvement efforts in the areas that matter most. Targeting high-risk and high complication rate procedures, NSQIP allows for better tracking, trending and high levels of data analysis. NSQIP participation also allows hospitals to collaborate on surgical care improvement while benchmarking like institutions.
The UCLA Health System Surgical Quality Team is very excited to begin participating in NSQIP. We will have more information about this great program posted soon. If you have questions or would like more information now, please contact our NSQIP Coordinator: hdash@mednet.ucla.edu
Publicly Reported Data/Collaboratives
HAC and PSI - More information about Hospital Acquired Conditions and Patient Safety Indicators can be found here.
Mortality
Readmissions